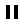Ankle sprains are remarkably common. In fact, one can argue that it may be the most common injury in the world. The vast majority of the time someone will “twist” an ankle, have a few days to a week of discomfort, and then return to normal activity. But there are times when this is not the case.
A sprain, by definition, is an injury to a ligament. And when one references an ankle sprain, it is usually the anterior talofibular ligament and/or the calcaneofibular ligament that is being referenced. Ankle sprains are graded to indicate either the severity of the tear or the number of ligaments involved. The treatment is generally guided by the well-known acronym R.I.C.E. Rest. Ice. Compression. Elevation. For severe sprains the support of a crutch may be needed. But even a severe ankle sprain will improve in three weeks.
Therefore, if someone has persistent pain and/or difficulty weeks or months after an ankle sprain, especially if there was difficulty bearing weight for more than three weeks after the injury, the problem may not be ‘just an ankle sprain’.
My Ankle Sprain Series will highlight 10+ injuries and approaches to treatment. Part One of this series covers the first three common “ankle sprain” injuries.
-
When you tear your Peroneal Tendons
The peroneal tendons are dynamic stabilizers of the ankle, and are important for stability as the terrain changes, and with activity. They work in concert with the ligaments, but are so much more, as they are intimately involved in Proprioception.
The peroneal tendons can be injured in the exact mechanism that sprains the lateral ankle ligaments; an inversion injury. The history is very similar, but patients report difficulty progressing, or a sense of weakness and difficulty on uneven ground. A detailed physical examination is key, as the examination will reveal tendon pain, as opposed to pain at the ligaments
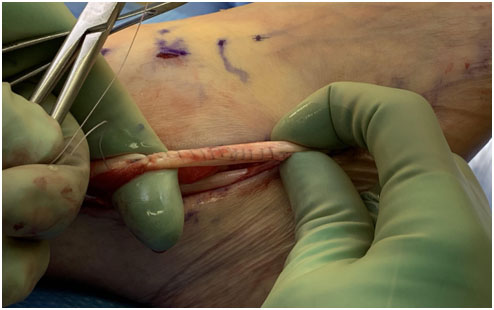
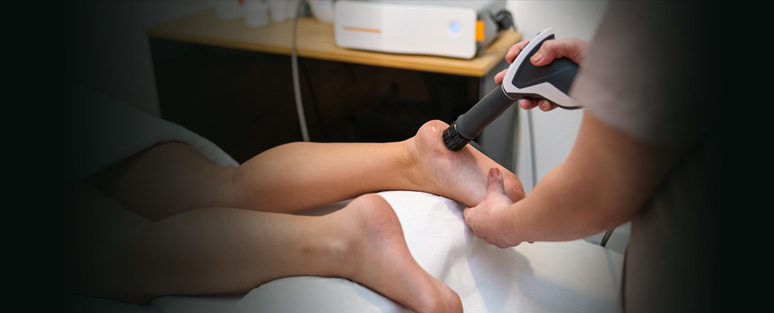
Although some believe that all tears should be repaired, small tears can be rehabilitated with physical therapy, and can do quite well without sequela. However, if therapy fails, or the tear is quite significant, symptoms may persist. Un-healed tears can result in persistent difficulty with activity requiring balance, quick adjustments, pivoting, rotation, and pain particularly going downstairs or downhill. Surgery may be needed.
The rehabilitation of these tendons is vital, whether the treatment is conservative or surgical.
-
When you have an unrecognized Achilles Tendon Rupture
In this particular case the tendon rupture was not recognized for a few months, requiring an Achilles Reconstruction, not just an Achilles Repair
Why is it masked?
Up to 25% of Achilles Tendon ruptures are unrecognized in the emergency room or urgent care, because they mimic ankle sprains in appearance and in the pattern of bruising. Interestingly enough, Achilles ruptures are not as painful as many assume, and so the severity of the injury may not register. It is also discounted because patients can still flex the ankle even though the Achilles is ruptured. However, an unrecognized Achilles Tendon Rupture severely impacts the function of the ankle.
Why does it matter?
The Achilles Tendon is the major ‘flexor’ of the ankle is responsible for picking the heel up off of the ground, and for power in push off when doing activities such as running or jumping. But it is also necessary for normal walking mechanics, and chronic heel pain can occur with every step if a rupture is unrecognized and becomes chronic. This Calcaneal Gait causes unrelenting heel pain with walking, and pressure changes can be seen in the plantar heel, as in the photo above. Cushioning of the heel becomes necessary to dampen pain with every step.
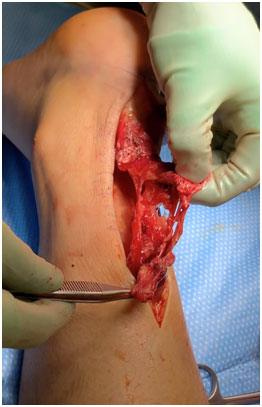
What to do?
When recognized early, it should be aggressively treated with either surgery, or if warranted, conservative care. When delayed, direct repair may not be possible, and it needs to be reconstructed to improve ankle function. I employ various reconstructive techniques depending on the size of the gap and the amount of tendon proximally and distally, one of which is demonstrated here. An absolutely shredded short Achilles Tendon rupture (shown here), required a fully open approach. You can see the full video on my IGTV channel. (@dr.main.girl)
It is important to differentiate a simple ankle sprain from a ruptured Achilles Tendon because routine walking becomes difficult, and running is impossible. A simple test, specific visual inspection and a good physical examination tells all.
-
When you have an unrecognized fracture of the lateral malleolus
What is the Lateral Malleolus?
It is lower end of the fibula, and is the bony projection on the outside of the ankle. It is the outer border of the ankle joint. The ankle ligaments attach to the end of the fibula and so the energy during a sprain can pass into the bone and result in a fracture.
Why can it be masked?
If the fracture is not severe, and is minimal, then the amount of swelling may be similar to a “bad ankle sprain”, though more bruising and swelling are expected. But some people mistake the pain with walking, with “ligament pain” and if they can push through the pain, they “tough it out”.
Why is it important?
When unrecognized, and patients are not immobilized and walk, then the fracture may have a difficult time healing, or may not heal, and result in persistent pain with walking, far beyond the normal healing time of an “ankle sprain”.
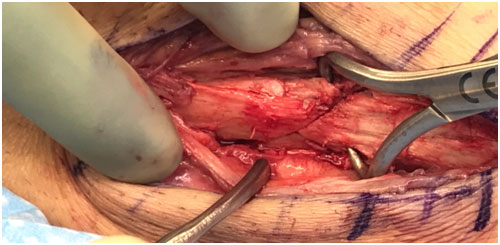
In this case, the patient came in to see me for persistent pain. X-rays demonstrated an unhealed fracture, and I diagnosed him with a non-union. The intraoperative photos can be graphic for some.
Check back here soon for more information on other common ankle injuries that aren’t just an Ankle Sprain.
Other Natalie S. Mesnier, MD Blogs: